AllergyHome is excited to introduce Karen S. Rance, DNP, RN, CPNP, AE-C. She is a leader in state and national initiatives addressing asthma and food allergy advocacy, education, and policy. Her many leadership roles and collaborations have served and continue to serve our community well. Thank you Dr. Rance for all that you do and thank you for joining us!
WHAT HAPPENS WHEN MY CHILD HAS MULTIPLE FOOD ALLERGIES?
Written by Karen Rance DNP, RN, CPNP,AE-C
Food allergies affect 6% of children and 3% to 4% of adults in the United States. For the child with food allergy, food allergen avoidance and readily accessible epinephrine injectors are the cornerstones of management. However, this becomes much more complicated when your child has multiple food allergies.
“The stress of having a child with multiple food allergies is real.”
 Because all of the major food allergens (peanut, milk, egg, soy, wheat, fish, shellfish, and tree nuts) are common in the American diet, food allergic children and their families often experience a significant negative impact on their quality of life. This effect is multiplied when more than one food allergy is involved. The stress of having a child with multiple food allergies is real. Studies show that the parents of children with multiple food allergies experience a greater loss in their quality of life than parents of children with only one food allergy. However when parents are armed with education and surrounded by a team of professionals (allergy team as well as others), the tasks at hand become achievable.
Because all of the major food allergens (peanut, milk, egg, soy, wheat, fish, shellfish, and tree nuts) are common in the American diet, food allergic children and their families often experience a significant negative impact on their quality of life. This effect is multiplied when more than one food allergy is involved. The stress of having a child with multiple food allergies is real. Studies show that the parents of children with multiple food allergies experience a greater loss in their quality of life than parents of children with only one food allergy. However when parents are armed with education and surrounded by a team of professionals (allergy team as well as others), the tasks at hand become achievable.
Consider growth and development, especially when dealing with multiple food allergies
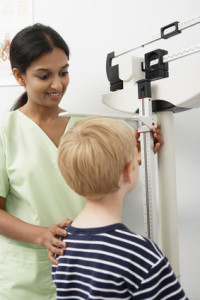 When your child is diagnosed with multiple food allergies, avoiding several food groups at the same time can be tricky and possibly have negative consequences on your child’s growth and development. Care is needed to ensure that your child has sufficient caloric intake and avoids developing a vitamin or mineral deficiency. Studies have found that children with milk allergy or multiple food allergies consumed less-than-recommended amounts of calcium compared with children without milk allergy and/or only one food allergy. Milk is not only an important source of calcium and vitamin D, but it also provides protein and fat. In this case, a suitable alternative to milk such as soy or almond milk (if tolerated) needs to be identified. For the most severely food allergic child, amino acid formula supplements (such as Elecare Jr.) provide a safe haven to ensure daily caloric need.
When your child is diagnosed with multiple food allergies, avoiding several food groups at the same time can be tricky and possibly have negative consequences on your child’s growth and development. Care is needed to ensure that your child has sufficient caloric intake and avoids developing a vitamin or mineral deficiency. Studies have found that children with milk allergy or multiple food allergies consumed less-than-recommended amounts of calcium compared with children without milk allergy and/or only one food allergy. Milk is not only an important source of calcium and vitamin D, but it also provides protein and fat. In this case, a suitable alternative to milk such as soy or almond milk (if tolerated) needs to be identified. For the most severely food allergic child, amino acid formula supplements (such as Elecare Jr.) provide a safe haven to ensure daily caloric need.
Making heads and tails of testing for multiple food allergies.
Depending on how many foods your child tested positive to, it may become necessary for your health care provider to prioritize the results to establish a step-wise plan for avoidance and follow up food challenge. The larger your child’s SPT result (i.e. wheals), the greater the likelihood that they will have an allergic reaction to that food. For example, if your child has a SPT result of at least 8 mm for milk or peanut and at least 7 mm for egg indicate a greater than 95% of an allergic reaction if that food is eaten. With blood testing, higher test results correlate to an increased likelihood of an allergic reaction. However, current testing cannot predict the severity of allergic reaction should it occur. All positive tests need to be taken in the context of history and viewed in relation to one another. Food challenges, when appropriate and performed under the direction of the allergy team, are a useful tool to confirm that a person can or can’t tolerate a particular food.
“It is important that children with multiple food allergies not limit their diet beyond the foods to which they have been diagnosed as being allergic.”
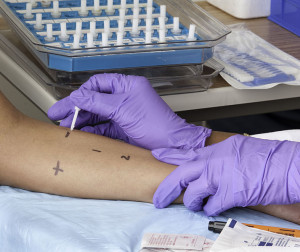 It is important that children with multiple food allergies not limit their diet beyond the foods to which they have been diagnosed as being allergic. It is common for families to be concerned about introducing other major food groups to their child despite having negative diagnostic tests to those particular foods or to avoid certain foods without having positive diagnostic tests. All of the foods that your child is avoiding need a proper diagnosis by means of an accurate history, either skin prick test (SPT) or immunoglobin E (IgE) blood tests, and potentially a food challenge.
It is important that children with multiple food allergies not limit their diet beyond the foods to which they have been diagnosed as being allergic. It is common for families to be concerned about introducing other major food groups to their child despite having negative diagnostic tests to those particular foods or to avoid certain foods without having positive diagnostic tests. All of the foods that your child is avoiding need a proper diagnosis by means of an accurate history, either skin prick test (SPT) or immunoglobin E (IgE) blood tests, and potentially a food challenge.
Use a team approach
 It is easy to become overwhelmed when asked to start and manage a food avoidance diet with multiple foods at the same time. Because of the many moving parts to this type of management, the avoidance of multiple foods is best accomplished with a multidisciplinary team; e.g. board certified allergist, nurse practitioner, registered dietician/nutritionist, nurse, occupational therapist, and/or mental health expert. If your child is diagnosed with multiple food allergies at a very young age their oromotor development can be affected. This occurs because there is a natural overlap between the time period when most major food groups are introduced (birth to 24 months) and the development of mature oral motor skills. Some children develop altered feeding behaviors because of repeated negative experiences associated with eating (such as vomiting, hives, or abdominal pain). This can be frustrating and result in food refusal, food aversion, or coughing/gagging in some cases. Your team of health care professionals can be a great help to your child in developing healthy feeding skills and developmentally appropriate feeding behavior.
It is easy to become overwhelmed when asked to start and manage a food avoidance diet with multiple foods at the same time. Because of the many moving parts to this type of management, the avoidance of multiple foods is best accomplished with a multidisciplinary team; e.g. board certified allergist, nurse practitioner, registered dietician/nutritionist, nurse, occupational therapist, and/or mental health expert. If your child is diagnosed with multiple food allergies at a very young age their oromotor development can be affected. This occurs because there is a natural overlap between the time period when most major food groups are introduced (birth to 24 months) and the development of mature oral motor skills. Some children develop altered feeding behaviors because of repeated negative experiences associated with eating (such as vomiting, hives, or abdominal pain). This can be frustrating and result in food refusal, food aversion, or coughing/gagging in some cases. Your team of health care professionals can be a great help to your child in developing healthy feeding skills and developmentally appropriate feeding behavior.
REFERENCES:
Cohen B, Noone S, Munoz-Furlong A, et al. Development of a questionnaire to measure quality of life in families with a child with food allergy. J Allergy Clin Immunol. 2004;114:1159–1163.
Flammarion S, Santos C, Guimber D, et al. A. Diet and nutritional status of children with food allergies. Ped Allergy Immunol. 2011;22(2), 161-165.
Sicherer S, Sampson H. Food allergy. J Allergy Clin Immunol. 2010;125(2), S116-S125.
Wang, J. Management of the patient with multiple food allergies. Current Allergy Asthma Reports. 2010;10(4), 271-277.
 Karen S. Rance, DNP, RN, CPNP, AE-C is an allergy, asthma, and immunology specialty NP who received her Doctorate in Nursing Practice from the University of Virginia. She received her Masters of Science in Nursing from Old Dominion University and her Bachelors of Science in Nursing from Vanderbilt University. She is in private practice at Allergy Partners of Central Indiana in Indianapolis. She is adjunct faculty at Indiana Wesleyan University, Graduate School of Nursing.
Karen S. Rance, DNP, RN, CPNP, AE-C is an allergy, asthma, and immunology specialty NP who received her Doctorate in Nursing Practice from the University of Virginia. She received her Masters of Science in Nursing from Old Dominion University and her Bachelors of Science in Nursing from Vanderbilt University. She is in private practice at Allergy Partners of Central Indiana in Indianapolis. She is adjunct faculty at Indiana Wesleyan University, Graduate School of Nursing.
Dr. Rance is the 2004 and 2011 recipient of the Allied Health Award for outstanding clinical project and the 2012 ARTrust mini-grant recipient for her leadership in implementing a statewide asthma management plan from the American Academy of Asthma, Allergy, and Immunology. She has presented at multiple national conferences on the topic of allergy and asthma, and regularly speaks to a broad spectrum of health care provider audiences on the topic of allergy and asthma. She has authored manuscripts for numerous medical journals including the Journal for Nurse Practitioners, Journal of Asthma and Allergy Educators, Journal of Pediatric Health Care, Journal of the American Academy of Nurse Practitioners, and Journal of Allergy and Clinical Immunology. Western Schools published her first course book, Management of Asthma in Adults and Children, in March 2014.
Dr. Rance serves on the Board of Directors of the National Association of Certified Asthma Educators (NAECB) and is on the National Heart, Lung, and Blood Institute (NHBLI)’s National Asthma Education Prevention Program Expert Panel (NAEPP) workgroup. She is the Founding Chair of the National Association of Pediatric Nurse Practitioners’ (NAPNAP) Asthma and Allergy Special Interest Group. She is on NAPNAP’s Clinical Expert Panel for Asthma. She is involved in many community support programs, including the Indiana Joint Asthma Coalition where she is directing the implementation of a statewide asthma action plan.
I am new to this blog. This is great Dr Rance. Do you have any nutritional guidelines for a 3 year old with egg , fish , nuts and garlic allergies?